tubingsebao
sebao 时间:2021-01-31 阅读:()
RESEARCHOpenAccessNasalcontinuouspositiveairwaypressureimprovesmyocardialperfusionreserveandendothelial-dependentvasodilationinpatientswithobstructivesleepapneaPatriciaKNguyen1*,ChandraKKatikireddy2,MichaelVMcConnell1,CleteKushida3,PhillipCYang1AbstractBackground:Obstructivesleepapnea(OSA)hasbeenassociatedwithcardiovasculardisease(CVD),butwhetherOSAisanindependentriskfactorforCVDiscontroversial.
ThepurposeofthisstudyistodetermineifpatientswithOSAhavesubclinicalcardiovasculardiseasethatisdetectablebymulti-modalitycardiovascularimagingandwhethertheseabnormalitiesimproveafternasalcontinuouspositiveairwaypressure(nCPAP).
Results:Ofthe35consecutivesubjectswithnewlydiagnosedmoderatetosevereOSArecruitedfromtheStanfordSleepDisordersClinic,20patientswererandomizedtoactivevs.
shamnCPAP.
ActivenCPAPwastitratedtopressuresthatwouldpreventsleepdisorderedbreathingbasedoninpatientpolysomnography.
OSApatientshadbaselinevascularfunctionabnormalitiesincludingdecreasedmyocardialperfusionreserve(MPR),brachialflowmediateddilation(FMD)andnitroglycerin-inducedcoronaryvasodilation.
PatientsrandomizedtoactivenCPAPhadimprovementofMPR(1.
5±0.
5vs.
3.
0±1.
3,p=0.
02)andbrachialFMD(2.
5%±5.
7%vs.
9.
0%±6.
5%,p=0.
03)aftertreatment,butthoserandomizedtoshamnCPAPshowednosignificantimprovement.
Therewerenosignificantchangesseeninchambersizes,systolicanddiastolicfunction,valvularfunctionandcoronaryvasodilationtonitroglycerin.
Conclusions:PatientswithmoderatetosevereOSAhaddecreasedMPRandbrachialFMDthatimprovedafter3monthsofnCPAP.
ThesefindingssuggestthatreliefofapneainOSAmayimprovemicrovasculardiseaseandendothelialdysfunction,whichmaypreventthedevelopmentofovertcardiovasculardisease.
Furtherstudyinalargerpatientpopulationmaybewarranted.
BackgroundObstructivesleepapnea(OSA)hasbeenassociatedwithanincreasedincidenceofcardiovasculardisease(CVD)andthesepatientsare,thus,likelytohaveahighburdenofsubclinicaldisease[1,2].
However,theextentofsub-clinicalCVDhasnotbeensystematicallyevaluated.
Previousstudieshaveusedsinglemeasuresofsubclinicaldisease[3-7].
Inaddition,whetherOSAplaysaninde-pendentroleinthedevelopmentofCVDremainscon-troversialsincemostpreviousstudiesarecrosssectionalandnotrandomized,and,thus,maynotadequatelycontrolforconfoundingfactors.
Weusemulti-modalitycardiovascularimaging(CVI)toevaluatesubclinicalCVDinpatientswithOSAbeforeandafterrandomizationtoactiveorshamnasalcontin-uouspositiveairwaypressure(nCPAP).
Wewill(1)determinethefrequencyofsubclinicalCVDusingmulti-modalityimaginginadultswithnewlydiagnosedmoderatetosevereOSAand(2)testthehypothesisthatnCPAPtherapy,thestandardtreatmentforOSA,improvestheseabnormalities.
*Correspondence:pnguyen@cvmed.
stanford.
edu1DepartmentofMedicine,DivisionofCardiovascularMedicine,StanfordUniversity,Stanford,CA,USAFulllistofauthorinformationisavailableattheendofthearticleNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/502010Nguyenetal;licenseeBioMedCentralLtd.
ThisisanOpenAccessarticledistributedunderthetermsoftheCreativeCommonsAttributionLicense(http://creativecommons.
org/licenses/by/2.
0),whichpermitsunrestricteduse,distribution,andreproductioninanymedium,providedtheoriginalworkisproperlycited.
MethodsSubjectsAtotalof35consecutivepatientswererecruitedfromthepatientpopulationseenattheStanfordSleepDisor-dersClinic.
Theinclusioncriteriainclude:1)newlydiag-nosedmoderatetosevereOSAasdefinedbytheAmericanAcademyofSleepMedicine[8],2)RDI≥15eventsperhourbyinpatientpolysomnography,and3)EpworthSleepinessScalescore>10.
Theexclusioncri-teriainclude:1)priortreatmentforOSA,2)anoxygensaturation10%ofthediagnosticsleepstudyor25%ofthefirst4hoursofthediagnosticsleepstudy,3)clinicalsymptomsordiagnosisofcoron-aryarterydisease,congestiveheartfailure,cardiacrhythmdisturbance,Raynaud'sdisease(whichisacon-traindicationforflowmediateddilation),respiratorydis-ease,diabetes,chronicneurologicaldisorders,cancernotinremission,andrenalfailure,4)metalobjects,devicesorimplantsinoronthebodyincludingpacemakers,aneurysmclips,prostheses,bullets,buckshot,shrapnel,andanymetalfragmentsfromworkingaroundmetal(whicharecontraindicationsforcardiovascularmagneticresonanceimaging)and5)contraindicationstoadeno-sineornitroglycerin.
Sevenparticipantsfailedtheinitialscreeningforeligibility,and8withdrewpriortorando-mization.
TheStanfordInstitutionalReviewBoardapprovedthestudy.
Allsubjectsgavewritteninformedconsent.
Recruitment,RandomizationandBlindingSubjectswereidentifiedforrecruitmentafterundergoingastandardovernightinpatientrespiratorypolysomno-graphicsleepstudy.
Thediagnosticpolysomnogramservedasthebaselinemeasure.
Patientsalsocompletedastandardquestionnairetoevaluatethedegreeofsleepi-nessandunderwentbaselineechocardiography,cardiacmagneticresonanceimaging,andvascularultrasound.
Afterbaselineassessments,subjectswererandomizedtoeitheractive(therapeutic)orsham(subtherapeutic)nCPAPandthenadmittedforasecondnightofpolysom-nographyfornCPAPtitration.
DuringthenCPAPtitra-tionnight,ifpatientswererandomizedtoactivenCPAP,pressureswerevariedthroughoutthenighttocontrolthepatients'sleepdisorderedbreathing.
ForthoseonshamnCPAP,pressuresfluctuatedslightlybutnomorethan0.
5cmH2Opressure,whichwasachievedbyinsertingaflowrestrictingconnectoratthemachineoutletandsixextra4mmholesinthecollarofthemaintubingattheendofthemasktoallowairtoescapeandtopreventre-breathingofcarbonmonoxide.
AcertifiedtechnicianreviewedthepolysomnogramsthenextdaytodeterminetheoptimaltherapeuticpressuretocontrolsnoringandsleepapneaforpatientsintheactivenCPAPgroup.
PatientsassignedtoshamnCPAPreceivedasimilarnCPAPdevicebutthemachinedeliveredairpressureinsufficienttopreventsleepdisorderedbreathing.
Inallotherways,thenCPAPmachinesweresimilar.
Thepatients,techniciansconductingthetitrationstudiesandinvestigatorsassessingtheimagingstudieswerenotawareoftreatmentgroupassignments.
Thus,thestudywaseffectivelydouble-blind.
Within7daysaftertheassessment,thepatientsweregiventheirnCPAPmachinesandinstructedhowtousethemachinesathome.
Studystaffcontactedpatientsmonthlytoassessadherencetothedevices.
Patientsreturnedafterthreemonthsforrepeatpolysomnogramandmulti-modalityCVIstudies.
Informationoncompli-ancewasdownloadedfromtheassignednCPAPmachinesattheendofthestudy.
PolysomnographyOvernightrespiratorypolysomnographicsleepstudieswereperformedatbaseline,fornCPAPtitration,andaftertreatment.
Anobstructedbreathingeventconsistedofanobstructiveapnea,hypopnea,orrespiratoryeffort-relatedarousals[9].
Moderateorsevereapneawasdefinedasarespiratorydisturbanceindex>15eventsperhourofsleep.
EchocardiographyEchocardiographicimageswereobtainedinstandardviewsbythesameexperiencedsonographer(HewlettPackard,Sonos,5500).
LeftventriculardiastolicfunctionandpulmonaryarterialpressurewasassessedbyDop-plerechocardiographyinaccordancewiththeAmericanSocietyofEchocardiographyrecommendations[10].
CardiovascularmagneticresonanceCardiovascularmagneticresonance(CMR)includedanassessmentofstructureandfunction,adenosinestressmyocardialperfusion,andcoronaryarteryvasodilationtonitroglycerin(NTG).
ImaginganalysiswasperformedusingReportCard,theGEsoftware.
Scanswereperformedusinga1.
5TSignaMRscanner(GEHealthcare,Milwaukee,WI)equippedwithhigh-performancegradients(40mT/m,150mT/m/ms).
Acommercial4-channelcardiacphased-arraysurfacecoilprovidedsignalreception(GEHealthcare,Milwau-kee,WI).
Areal-timeinteractivesystem(iDrive,GEHealthcare,Milwaukee,WI)wasusedforlocalization.
AssessmentofcardiacfunctionwasobtainedusinganECG-triggeredretrospectivelygatedcineSSFPsequence(20phasespercardiaccycle,TR=3.
6ms,TE=1.
6ms,FOV=280to390mmandflipangle=40°).
First-passmyocardialperfusionimagingwasperformedusingasegmentedecho-planarimagingpulsesequencewithaNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page2of10notchedsaturationpulse[11].
Forstressimaging,adeno-sinewasadministeredintravenouslyatarateof140mcg/kg/minfor4minutes,followedbyfirst-passmyocardialperfusionimagingduringintravenousinjec-tionof0.
1mmol/kggadolinium-DPTAatarateof5ml/s.
Restperfusionimageswereacquiredapproxi-mately10minutesafterstressimages.
Thefollowingperfusionpulsesequenceparameterswereused:TR=2.
4ms,TE=1.
2ms,inversiontime=158to211ms,echotrainlength=4to8ms,FOV=34to37*25to27cm,matrix=128*128,flipangle=25°,andslicethickness=10mm.
Therestperfusionimagesweregenerallyacquiredwiththesamegraphicprescriptionusedforthestressimages.
Foranalysisofmyocardialperfusion,signalintensitywasdeterminedforeachofthethreecontiguousslicesrepresentingthebase,midandapexoftheleftventricle.
Thesignalintensitybeforecontrastagentadministrationwassubtracted,andtheupslopeoftheresultingsignalintensitytimecurvewasdetermined.
Aperfusionscorewasgeneratedbyaddingtheupslopeofeachofthethreeslices.
Themyocardialperfusionreserve(MPR)wascalculatedastheratiobetweenthemyocardialperfusionscoreatstressdividedbythemyocardialperfusionscoreatrest.
NTG-inducedcoronaryvasodilationwasthenper-formed.
Usingareal-timeinteractivesystem,in-planeviewsoftherightcoronaryartery(RCA)wereprescribed.
Across-sectionalviewofthemostlinearportionoftheproximaltomidRCAwasprescribed.
Multi-slicehigh-resolutionspiralcoronarymagneticresonanceangiogra-phywasperformedwithcardiacgating,breath-holding,andacquisitionduringdiastole(FOV=22cm,in-planespatialresolution=0.
7mm,slicethickness=5mm,3slices,TR=1heartbeat,TE=2.
5ms,18interleaves,andflipangle=60°).
Cross-sectionalspiralhigh-resolu-tioncoronarymagneticresonanceangiographyimages[12]wereacquiredbeforeand5minutesafteradminis-trationof0.
4mgsublingualNTGwhilethepatientwasinsidethemagnet.
Usingthecross-sectionalRCAimages,themostcircu-larandcorrespondingsliceswereidentifiedonthepre-andpost-NTGimages.
Theseimageswereallpooledandthenrandomized,withneitherpatientnorNTGinformationprovidedontheimages.
Weusedacustomdesignedsoftwareprogramtoanalyzethecrosssectionalimages.
Imagesweremagnifiedtwo-fold,andanovoidregionofinteresttoolwasusedtotracearoundtheRCA,yieldingthecross-sectionalarea.
VascularUltrasoundEndothelialfunctionwasassessednon-invasivelyusingvascularultrasoundtomeasurebrachialarteryflowmediateddilation(FMD)followingreactivehyperemiainaccordancewithpublishedguidelines[13].
Studieswereperformedbyoneoftwotrainedoperators.
Studieswereperformedatthesametimeofdayandinthefast-ingstate.
Vasoactivemedicationswereheld24hourspriortothestudy.
Brachialarterydiametersweremeasuredusinganautomatedsoftwaresystemtodetectnearandfarwalledgesandmeasurevesseldiameterforeachframeinthe10-secondloop(VascularAnalysisTools,MedicalIma-gingApplications,Iowa,USA).
Allanalyseswereper-formedbyoneoftwotrainedoperators.
Previousreproducibilitystudiesindicatehighoperatoragreement.
SampleSizeCalculationThesamplesizewasestimatedbasedonapreviousran-domizedstudycomparingFMDinpatientswithmoder-atetosevereOSArandomizedto3monthsofnCPAPandnonCPAP[14].
FMDwassignificantlylowerinpatientsrandomizedtonCPAP(nCPAP8.
9±1.
9%,nonCPAP5.
0±0.
7%,p=0.
02).
Usingatwotaileda=0.
01andpowerof0.
90,anattritionrateof20%,theesti-matedsamplesizeis10subjectspereachgroup(totalnumberofsubjectsis20).
StatisticalAnalysisContinuousvariableswerereportedasmeanswithstan-darddeviations.
Categoricalvariableswerereportedasfrequenciesandcounts.
Standardthresholdsforabnor-malvalueswereusedforallparameters.
AnMPR70%)hadaflowreservelessthan2.
5[15].
AnMPRof0.
75and1cm/s10%(1/10)0%(0/10)10%(1/10)20%(2/10)pvalue1.
01.
01.
00.
25E/Aratio≤0.
7540%(4/10)10%(1/10)0%(0/10)20%(2/10)>0.
75&240ms40%(4/10)20%(2/10)10%(1/10)30%(3/10)pvalue0.
620.
331.
001.
00E'≤8cm/s11%(1/9)20%(2/10)11%(1/9)40%(4/10)>8cm/s89%(8/9)80%(8/10)89%(8/9)60%(6/10)pvalue0.
920.
301.
000.
25E/e'150%(0/10)0%(0/10)0%(0/10)0%(0/10)pvalue0.
900.
660.
50.
5S/DratioS>D50%(4/8)40%(2/5)5/8(50%)40%(2/5)S=D50%(4/8)60%(3/5)3/8(30%)60%(3/5)SSebaounS,BlochE,Orvoen-FrijaE,OppertJM,HuchonG:Leftventricularsystolicdysfunctioninpatientswithobstructivesleepapneasyndrome.
Chest2002,122(4):1133-8.
19.
Romero-CorralA,SomersVK,PellikkaPA,OlsonEJ,BaileyKR,KorinekJ,OrbanM,Sierra-JohnsonJ,KatoM,AminRS,Lopez-JimenezF:Decreasedrightandleftventricularmyocardialperformanceinobstructivesleepapnea.
Chest2007,132(6):1863-70.
20.
ChamiHA,DevereuxRB,GottdienerJS,MehraR,RomanMJ,BenjaminEJ,GottliebDJ:Leftventricularmorphologyandsystolicfunctioninsleep-disorderedbreathing:theSleepHeartHealthStudy.
Circulation2008,117(20):2599-607.
21.
SannerBM,KonermannM,SturmA,MullerHJ,ZidekW:Rightventriculardysfunctioninpatientswithobstructivesleepapnoeasyndrome.
EuropeanRespiratoryJournal1997,10(9):2079-83.
22.
DursunogluD,DursunogluN,EvrengulH,OzkurtS,KuruO,KilicM,FisekciF:Impactofobstructivesleepapnoeaonleftventricularmassandglobalfunction.
EurRespiratoryJournal2005,26(2):283-8.
23.
NiroumandM,KupersteinR,SassonZ,HanlyPJ:Impactofobstructivesleepapneaonleftventricularmassanddiastolicfunction.
AmericanJournalofRespiratoryandCriticalCareMedicine2001,163(7):1632-6.
24.
AlchanatisM,TourkohoritiG,KakourosS,KosmasE,PodarasS,JordanoglouJB:Daytimepulmonaryhypertensioninpatientswithobstructivesleepapnea:theeffectofcontinuouspositiveairwaypressureonpulmonaryhemodynamics.
Respiration;InternationalReviewofThoracicDiseases2001,68(6):566-72.
25.
ShivalkarB,VandeHeyningC,KerremansM,RinkevichD,VerbraeckenJ,DeBackerW,VrintsC:Obstructivesleepapneasyndrome:moreinsightsonstructuralandfunctionalcardiacalterations,andtheeffectsoftreatmentwithcontinuouspositiveairwaypressure.
JournaloftheAmericanCollegeofCardiology2006,47(7):1433-9.
26.
KaufmannPA,Gnecchi-RusconeT,diTerlizziM,SchafersKP,LuscherTF,CamiciPG:Coronaryheartdiseaseinsmokers:vitaminCrestorescoronarymicrocirculatoryfunction.
Circulation2000,102(11):1233-8.
27.
DayanikliF,GrambowD,MuzikO,MoscaL,RubenfireM,SchwaigerM:Earlydetectionofabnormalcoronaryflowreserveinasymptomaticmenathighriskforcoronaryarterydiseaseusingpositronemissiontomography.
Circulation1994,90(2):808-17.
28.
GouldKL,MartucciJP,GoldbergDI,HessMJ,EdensRP,LatifiR,DudrickSJ:Short-termcholesterolloweringdecreasessizeandseverityofperfusionabnormalitiesbypositronemissiontomographyafterdipyridamoleinpatientswithcoronaryarterydisease.
Apotentialnoninvasivemarkerofhealingcoronaryendothelium.
Circulation1994,89(4):1530-8.
Nguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page9of1029.
CarlsonJT,RangemarkC,HednerJA:Attenuatedendothelium-dependentvascularrelaxationinpatientswithsleepapnoea.
JournalofHypertension1996,14(5):577-84.
30.
KatoM,Roberts-ThomsonP,PhillipsBG,HaynesWG,WinnickiM,AccursoV,SomersVK:Impairmentofendothelium-dependentvasodilationofresistancevesselsinpatientswithobstructivesleepapnea.
Circulation2000,102(21):2607-10.
31.
LattimoreJL,WilcoxI,SkiltonM,LangenfeldM,CelermajerDS:Treatmentofobstructivesleepapnoealeadstoimprovedmicrovascularendothelialfunctioninthesystemiccirculation.
Thorax2006,61(6):491-5.
32.
ImadojemuVA,GleesonK,QuraishiSA,KunselmanAR,SinowayLI,LeuenbergerUA:Impairedvasodilatorresponsesinobstructivesleepapneaareimprovedwithcontinuouspositiveairwaypressuretherapy.
AmericanJournalofRespiratoryandCriticalCareMedicine2002,165(7):950-3.
33.
IpMS,LamB,ChanLY,ZhengL,TsangKW,FungPC,LamWK:Circulatingnitricoxideissuppressedinobstructivesleepapneaandisreversedbynasalcontinuouspositiveairwaypressure.
AmericanJournalofRespiratoryandCriticalCareMedicine2000,162(6):2166-71.
34.
LanfranchiP,SomersVK:Obstructivesleepapneaandvasculardisease.
RespiratoryResearch2001,2(6):315-9.
35.
Orea-TejedaA,Valencia-FloresM,Castillo-MartinezL,Rebollar-GonzalezV,Gonzalez-BarrancoJ,CastanoA,AsensioE,Dorantes-GarciaJ,Sepulveda-MendezJ,Oseguera-MoguelJ,Garcia-RamosG,CanoA:AbnormalSPECTmyocardialperfusionimagingduringperiodsofobstructivesleepapneainmorbidobesepatientswithoutknownheartdisease.
ReviewofClinicalInvestigation2003,55(1):18-25.
36.
CerielloA,MotzE:Isoxidativestressthepathogenicmechanismunderlyinginsulinresistance,diabetes,andcardiovasculardiseaseThecommonsoilhypothesisrevisited.
Arteriosclerosis,thrombosis,andvascularbiology2004,24(5):816-23.
37.
HillJM,ZalosG,HalcoxJ,ShenkeW,WaclawiwM,QuyyumiAA,FinkelT:Circulatingendothelialcells,vascularfunction,andcardiovascularrisk.
NewEnglandJournalofMedicine2003,348:593-600.
38.
WangJ,SimAS,WangXL,WilckenDE:L-arginineregulatesasymmetricdimethylargininemetabolismbyinhibitingdimethylargininedimethylaminohydrolaseactivityinhepatic(HepG2)cells.
CellularandMolecularLifeSciences2006,63(23):2838-46.
doi:10.
1186/1532-429X-12-50Citethisarticleas:Nguyenetal.
:Nasalcontinuouspositiveairwaypressureimprovesmyocardialperfusionreserveandendothelial-dependentvasodilationinpatientswithobstructivesleepapnea.
JournalofCardiovascularMagneticResonance201012:50.
SubmityournextmanuscripttoBioMedCentralandtakefulladvantageof:ConvenientonlinesubmissionThoroughpeerreviewNospaceconstraintsorcolorgurechargesImmediatepublicationonacceptanceInclusioninPubMed,CAS,ScopusandGoogleScholarResearchwhichisfreelyavailableforredistributionSubmityourmanuscriptatwww.
biomedcentral.
com/submitNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page10of10
ThepurposeofthisstudyistodetermineifpatientswithOSAhavesubclinicalcardiovasculardiseasethatisdetectablebymulti-modalitycardiovascularimagingandwhethertheseabnormalitiesimproveafternasalcontinuouspositiveairwaypressure(nCPAP).
Results:Ofthe35consecutivesubjectswithnewlydiagnosedmoderatetosevereOSArecruitedfromtheStanfordSleepDisordersClinic,20patientswererandomizedtoactivevs.
shamnCPAP.
ActivenCPAPwastitratedtopressuresthatwouldpreventsleepdisorderedbreathingbasedoninpatientpolysomnography.
OSApatientshadbaselinevascularfunctionabnormalitiesincludingdecreasedmyocardialperfusionreserve(MPR),brachialflowmediateddilation(FMD)andnitroglycerin-inducedcoronaryvasodilation.
PatientsrandomizedtoactivenCPAPhadimprovementofMPR(1.
5±0.
5vs.
3.
0±1.
3,p=0.
02)andbrachialFMD(2.
5%±5.
7%vs.
9.
0%±6.
5%,p=0.
03)aftertreatment,butthoserandomizedtoshamnCPAPshowednosignificantimprovement.
Therewerenosignificantchangesseeninchambersizes,systolicanddiastolicfunction,valvularfunctionandcoronaryvasodilationtonitroglycerin.
Conclusions:PatientswithmoderatetosevereOSAhaddecreasedMPRandbrachialFMDthatimprovedafter3monthsofnCPAP.
ThesefindingssuggestthatreliefofapneainOSAmayimprovemicrovasculardiseaseandendothelialdysfunction,whichmaypreventthedevelopmentofovertcardiovasculardisease.
Furtherstudyinalargerpatientpopulationmaybewarranted.
BackgroundObstructivesleepapnea(OSA)hasbeenassociatedwithanincreasedincidenceofcardiovasculardisease(CVD)andthesepatientsare,thus,likelytohaveahighburdenofsubclinicaldisease[1,2].
However,theextentofsub-clinicalCVDhasnotbeensystematicallyevaluated.
Previousstudieshaveusedsinglemeasuresofsubclinicaldisease[3-7].
Inaddition,whetherOSAplaysaninde-pendentroleinthedevelopmentofCVDremainscon-troversialsincemostpreviousstudiesarecrosssectionalandnotrandomized,and,thus,maynotadequatelycontrolforconfoundingfactors.
Weusemulti-modalitycardiovascularimaging(CVI)toevaluatesubclinicalCVDinpatientswithOSAbeforeandafterrandomizationtoactiveorshamnasalcontin-uouspositiveairwaypressure(nCPAP).
Wewill(1)determinethefrequencyofsubclinicalCVDusingmulti-modalityimaginginadultswithnewlydiagnosedmoderatetosevereOSAand(2)testthehypothesisthatnCPAPtherapy,thestandardtreatmentforOSA,improvestheseabnormalities.
*Correspondence:pnguyen@cvmed.
stanford.
edu1DepartmentofMedicine,DivisionofCardiovascularMedicine,StanfordUniversity,Stanford,CA,USAFulllistofauthorinformationisavailableattheendofthearticleNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/502010Nguyenetal;licenseeBioMedCentralLtd.
ThisisanOpenAccessarticledistributedunderthetermsoftheCreativeCommonsAttributionLicense(http://creativecommons.
org/licenses/by/2.
0),whichpermitsunrestricteduse,distribution,andreproductioninanymedium,providedtheoriginalworkisproperlycited.
MethodsSubjectsAtotalof35consecutivepatientswererecruitedfromthepatientpopulationseenattheStanfordSleepDisor-dersClinic.
Theinclusioncriteriainclude:1)newlydiag-nosedmoderatetosevereOSAasdefinedbytheAmericanAcademyofSleepMedicine[8],2)RDI≥15eventsperhourbyinpatientpolysomnography,and3)EpworthSleepinessScalescore>10.
Theexclusioncri-teriainclude:1)priortreatmentforOSA,2)anoxygensaturation10%ofthediagnosticsleepstudyor25%ofthefirst4hoursofthediagnosticsleepstudy,3)clinicalsymptomsordiagnosisofcoron-aryarterydisease,congestiveheartfailure,cardiacrhythmdisturbance,Raynaud'sdisease(whichisacon-traindicationforflowmediateddilation),respiratorydis-ease,diabetes,chronicneurologicaldisorders,cancernotinremission,andrenalfailure,4)metalobjects,devicesorimplantsinoronthebodyincludingpacemakers,aneurysmclips,prostheses,bullets,buckshot,shrapnel,andanymetalfragmentsfromworkingaroundmetal(whicharecontraindicationsforcardiovascularmagneticresonanceimaging)and5)contraindicationstoadeno-sineornitroglycerin.
Sevenparticipantsfailedtheinitialscreeningforeligibility,and8withdrewpriortorando-mization.
TheStanfordInstitutionalReviewBoardapprovedthestudy.
Allsubjectsgavewritteninformedconsent.
Recruitment,RandomizationandBlindingSubjectswereidentifiedforrecruitmentafterundergoingastandardovernightinpatientrespiratorypolysomno-graphicsleepstudy.
Thediagnosticpolysomnogramservedasthebaselinemeasure.
Patientsalsocompletedastandardquestionnairetoevaluatethedegreeofsleepi-nessandunderwentbaselineechocardiography,cardiacmagneticresonanceimaging,andvascularultrasound.
Afterbaselineassessments,subjectswererandomizedtoeitheractive(therapeutic)orsham(subtherapeutic)nCPAPandthenadmittedforasecondnightofpolysom-nographyfornCPAPtitration.
DuringthenCPAPtitra-tionnight,ifpatientswererandomizedtoactivenCPAP,pressureswerevariedthroughoutthenighttocontrolthepatients'sleepdisorderedbreathing.
ForthoseonshamnCPAP,pressuresfluctuatedslightlybutnomorethan0.
5cmH2Opressure,whichwasachievedbyinsertingaflowrestrictingconnectoratthemachineoutletandsixextra4mmholesinthecollarofthemaintubingattheendofthemasktoallowairtoescapeandtopreventre-breathingofcarbonmonoxide.
AcertifiedtechnicianreviewedthepolysomnogramsthenextdaytodeterminetheoptimaltherapeuticpressuretocontrolsnoringandsleepapneaforpatientsintheactivenCPAPgroup.
PatientsassignedtoshamnCPAPreceivedasimilarnCPAPdevicebutthemachinedeliveredairpressureinsufficienttopreventsleepdisorderedbreathing.
Inallotherways,thenCPAPmachinesweresimilar.
Thepatients,techniciansconductingthetitrationstudiesandinvestigatorsassessingtheimagingstudieswerenotawareoftreatmentgroupassignments.
Thus,thestudywaseffectivelydouble-blind.
Within7daysaftertheassessment,thepatientsweregiventheirnCPAPmachinesandinstructedhowtousethemachinesathome.
Studystaffcontactedpatientsmonthlytoassessadherencetothedevices.
Patientsreturnedafterthreemonthsforrepeatpolysomnogramandmulti-modalityCVIstudies.
Informationoncompli-ancewasdownloadedfromtheassignednCPAPmachinesattheendofthestudy.
PolysomnographyOvernightrespiratorypolysomnographicsleepstudieswereperformedatbaseline,fornCPAPtitration,andaftertreatment.
Anobstructedbreathingeventconsistedofanobstructiveapnea,hypopnea,orrespiratoryeffort-relatedarousals[9].
Moderateorsevereapneawasdefinedasarespiratorydisturbanceindex>15eventsperhourofsleep.
EchocardiographyEchocardiographicimageswereobtainedinstandardviewsbythesameexperiencedsonographer(HewlettPackard,Sonos,5500).
LeftventriculardiastolicfunctionandpulmonaryarterialpressurewasassessedbyDop-plerechocardiographyinaccordancewiththeAmericanSocietyofEchocardiographyrecommendations[10].
CardiovascularmagneticresonanceCardiovascularmagneticresonance(CMR)includedanassessmentofstructureandfunction,adenosinestressmyocardialperfusion,andcoronaryarteryvasodilationtonitroglycerin(NTG).
ImaginganalysiswasperformedusingReportCard,theGEsoftware.
Scanswereperformedusinga1.
5TSignaMRscanner(GEHealthcare,Milwaukee,WI)equippedwithhigh-performancegradients(40mT/m,150mT/m/ms).
Acommercial4-channelcardiacphased-arraysurfacecoilprovidedsignalreception(GEHealthcare,Milwau-kee,WI).
Areal-timeinteractivesystem(iDrive,GEHealthcare,Milwaukee,WI)wasusedforlocalization.
AssessmentofcardiacfunctionwasobtainedusinganECG-triggeredretrospectivelygatedcineSSFPsequence(20phasespercardiaccycle,TR=3.
6ms,TE=1.
6ms,FOV=280to390mmandflipangle=40°).
First-passmyocardialperfusionimagingwasperformedusingasegmentedecho-planarimagingpulsesequencewithaNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page2of10notchedsaturationpulse[11].
Forstressimaging,adeno-sinewasadministeredintravenouslyatarateof140mcg/kg/minfor4minutes,followedbyfirst-passmyocardialperfusionimagingduringintravenousinjec-tionof0.
1mmol/kggadolinium-DPTAatarateof5ml/s.
Restperfusionimageswereacquiredapproxi-mately10minutesafterstressimages.
Thefollowingperfusionpulsesequenceparameterswereused:TR=2.
4ms,TE=1.
2ms,inversiontime=158to211ms,echotrainlength=4to8ms,FOV=34to37*25to27cm,matrix=128*128,flipangle=25°,andslicethickness=10mm.
Therestperfusionimagesweregenerallyacquiredwiththesamegraphicprescriptionusedforthestressimages.
Foranalysisofmyocardialperfusion,signalintensitywasdeterminedforeachofthethreecontiguousslicesrepresentingthebase,midandapexoftheleftventricle.
Thesignalintensitybeforecontrastagentadministrationwassubtracted,andtheupslopeoftheresultingsignalintensitytimecurvewasdetermined.
Aperfusionscorewasgeneratedbyaddingtheupslopeofeachofthethreeslices.
Themyocardialperfusionreserve(MPR)wascalculatedastheratiobetweenthemyocardialperfusionscoreatstressdividedbythemyocardialperfusionscoreatrest.
NTG-inducedcoronaryvasodilationwasthenper-formed.
Usingareal-timeinteractivesystem,in-planeviewsoftherightcoronaryartery(RCA)wereprescribed.
Across-sectionalviewofthemostlinearportionoftheproximaltomidRCAwasprescribed.
Multi-slicehigh-resolutionspiralcoronarymagneticresonanceangiogra-phywasperformedwithcardiacgating,breath-holding,andacquisitionduringdiastole(FOV=22cm,in-planespatialresolution=0.
7mm,slicethickness=5mm,3slices,TR=1heartbeat,TE=2.
5ms,18interleaves,andflipangle=60°).
Cross-sectionalspiralhigh-resolu-tioncoronarymagneticresonanceangiographyimages[12]wereacquiredbeforeand5minutesafteradminis-trationof0.
4mgsublingualNTGwhilethepatientwasinsidethemagnet.
Usingthecross-sectionalRCAimages,themostcircu-larandcorrespondingsliceswereidentifiedonthepre-andpost-NTGimages.
Theseimageswereallpooledandthenrandomized,withneitherpatientnorNTGinformationprovidedontheimages.
Weusedacustomdesignedsoftwareprogramtoanalyzethecrosssectionalimages.
Imagesweremagnifiedtwo-fold,andanovoidregionofinteresttoolwasusedtotracearoundtheRCA,yieldingthecross-sectionalarea.
VascularUltrasoundEndothelialfunctionwasassessednon-invasivelyusingvascularultrasoundtomeasurebrachialarteryflowmediateddilation(FMD)followingreactivehyperemiainaccordancewithpublishedguidelines[13].
Studieswereperformedbyoneoftwotrainedoperators.
Studieswereperformedatthesametimeofdayandinthefast-ingstate.
Vasoactivemedicationswereheld24hourspriortothestudy.
Brachialarterydiametersweremeasuredusinganautomatedsoftwaresystemtodetectnearandfarwalledgesandmeasurevesseldiameterforeachframeinthe10-secondloop(VascularAnalysisTools,MedicalIma-gingApplications,Iowa,USA).
Allanalyseswereper-formedbyoneoftwotrainedoperators.
Previousreproducibilitystudiesindicatehighoperatoragreement.
SampleSizeCalculationThesamplesizewasestimatedbasedonapreviousran-domizedstudycomparingFMDinpatientswithmoder-atetosevereOSArandomizedto3monthsofnCPAPandnonCPAP[14].
FMDwassignificantlylowerinpatientsrandomizedtonCPAP(nCPAP8.
9±1.
9%,nonCPAP5.
0±0.
7%,p=0.
02).
Usingatwotaileda=0.
01andpowerof0.
90,anattritionrateof20%,theesti-matedsamplesizeis10subjectspereachgroup(totalnumberofsubjectsis20).
StatisticalAnalysisContinuousvariableswerereportedasmeanswithstan-darddeviations.
Categoricalvariableswerereportedasfrequenciesandcounts.
Standardthresholdsforabnor-malvalueswereusedforallparameters.
AnMPR70%)hadaflowreservelessthan2.
5[15].
AnMPRof0.
75and1cm/s10%(1/10)0%(0/10)10%(1/10)20%(2/10)pvalue1.
01.
01.
00.
25E/Aratio≤0.
7540%(4/10)10%(1/10)0%(0/10)20%(2/10)>0.
75&240ms40%(4/10)20%(2/10)10%(1/10)30%(3/10)pvalue0.
620.
331.
001.
00E'≤8cm/s11%(1/9)20%(2/10)11%(1/9)40%(4/10)>8cm/s89%(8/9)80%(8/10)89%(8/9)60%(6/10)pvalue0.
920.
301.
000.
25E/e'150%(0/10)0%(0/10)0%(0/10)0%(0/10)pvalue0.
900.
660.
50.
5S/DratioS>D50%(4/8)40%(2/5)5/8(50%)40%(2/5)S=D50%(4/8)60%(3/5)3/8(30%)60%(3/5)SSebaounS,BlochE,Orvoen-FrijaE,OppertJM,HuchonG:Leftventricularsystolicdysfunctioninpatientswithobstructivesleepapneasyndrome.
Chest2002,122(4):1133-8.
19.
Romero-CorralA,SomersVK,PellikkaPA,OlsonEJ,BaileyKR,KorinekJ,OrbanM,Sierra-JohnsonJ,KatoM,AminRS,Lopez-JimenezF:Decreasedrightandleftventricularmyocardialperformanceinobstructivesleepapnea.
Chest2007,132(6):1863-70.
20.
ChamiHA,DevereuxRB,GottdienerJS,MehraR,RomanMJ,BenjaminEJ,GottliebDJ:Leftventricularmorphologyandsystolicfunctioninsleep-disorderedbreathing:theSleepHeartHealthStudy.
Circulation2008,117(20):2599-607.
21.
SannerBM,KonermannM,SturmA,MullerHJ,ZidekW:Rightventriculardysfunctioninpatientswithobstructivesleepapnoeasyndrome.
EuropeanRespiratoryJournal1997,10(9):2079-83.
22.
DursunogluD,DursunogluN,EvrengulH,OzkurtS,KuruO,KilicM,FisekciF:Impactofobstructivesleepapnoeaonleftventricularmassandglobalfunction.
EurRespiratoryJournal2005,26(2):283-8.
23.
NiroumandM,KupersteinR,SassonZ,HanlyPJ:Impactofobstructivesleepapneaonleftventricularmassanddiastolicfunction.
AmericanJournalofRespiratoryandCriticalCareMedicine2001,163(7):1632-6.
24.
AlchanatisM,TourkohoritiG,KakourosS,KosmasE,PodarasS,JordanoglouJB:Daytimepulmonaryhypertensioninpatientswithobstructivesleepapnea:theeffectofcontinuouspositiveairwaypressureonpulmonaryhemodynamics.
Respiration;InternationalReviewofThoracicDiseases2001,68(6):566-72.
25.
ShivalkarB,VandeHeyningC,KerremansM,RinkevichD,VerbraeckenJ,DeBackerW,VrintsC:Obstructivesleepapneasyndrome:moreinsightsonstructuralandfunctionalcardiacalterations,andtheeffectsoftreatmentwithcontinuouspositiveairwaypressure.
JournaloftheAmericanCollegeofCardiology2006,47(7):1433-9.
26.
KaufmannPA,Gnecchi-RusconeT,diTerlizziM,SchafersKP,LuscherTF,CamiciPG:Coronaryheartdiseaseinsmokers:vitaminCrestorescoronarymicrocirculatoryfunction.
Circulation2000,102(11):1233-8.
27.
DayanikliF,GrambowD,MuzikO,MoscaL,RubenfireM,SchwaigerM:Earlydetectionofabnormalcoronaryflowreserveinasymptomaticmenathighriskforcoronaryarterydiseaseusingpositronemissiontomography.
Circulation1994,90(2):808-17.
28.
GouldKL,MartucciJP,GoldbergDI,HessMJ,EdensRP,LatifiR,DudrickSJ:Short-termcholesterolloweringdecreasessizeandseverityofperfusionabnormalitiesbypositronemissiontomographyafterdipyridamoleinpatientswithcoronaryarterydisease.
Apotentialnoninvasivemarkerofhealingcoronaryendothelium.
Circulation1994,89(4):1530-8.
Nguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page9of1029.
CarlsonJT,RangemarkC,HednerJA:Attenuatedendothelium-dependentvascularrelaxationinpatientswithsleepapnoea.
JournalofHypertension1996,14(5):577-84.
30.
KatoM,Roberts-ThomsonP,PhillipsBG,HaynesWG,WinnickiM,AccursoV,SomersVK:Impairmentofendothelium-dependentvasodilationofresistancevesselsinpatientswithobstructivesleepapnea.
Circulation2000,102(21):2607-10.
31.
LattimoreJL,WilcoxI,SkiltonM,LangenfeldM,CelermajerDS:Treatmentofobstructivesleepapnoealeadstoimprovedmicrovascularendothelialfunctioninthesystemiccirculation.
Thorax2006,61(6):491-5.
32.
ImadojemuVA,GleesonK,QuraishiSA,KunselmanAR,SinowayLI,LeuenbergerUA:Impairedvasodilatorresponsesinobstructivesleepapneaareimprovedwithcontinuouspositiveairwaypressuretherapy.
AmericanJournalofRespiratoryandCriticalCareMedicine2002,165(7):950-3.
33.
IpMS,LamB,ChanLY,ZhengL,TsangKW,FungPC,LamWK:Circulatingnitricoxideissuppressedinobstructivesleepapneaandisreversedbynasalcontinuouspositiveairwaypressure.
AmericanJournalofRespiratoryandCriticalCareMedicine2000,162(6):2166-71.
34.
LanfranchiP,SomersVK:Obstructivesleepapneaandvasculardisease.
RespiratoryResearch2001,2(6):315-9.
35.
Orea-TejedaA,Valencia-FloresM,Castillo-MartinezL,Rebollar-GonzalezV,Gonzalez-BarrancoJ,CastanoA,AsensioE,Dorantes-GarciaJ,Sepulveda-MendezJ,Oseguera-MoguelJ,Garcia-RamosG,CanoA:AbnormalSPECTmyocardialperfusionimagingduringperiodsofobstructivesleepapneainmorbidobesepatientswithoutknownheartdisease.
ReviewofClinicalInvestigation2003,55(1):18-25.
36.
CerielloA,MotzE:Isoxidativestressthepathogenicmechanismunderlyinginsulinresistance,diabetes,andcardiovasculardiseaseThecommonsoilhypothesisrevisited.
Arteriosclerosis,thrombosis,andvascularbiology2004,24(5):816-23.
37.
HillJM,ZalosG,HalcoxJ,ShenkeW,WaclawiwM,QuyyumiAA,FinkelT:Circulatingendothelialcells,vascularfunction,andcardiovascularrisk.
NewEnglandJournalofMedicine2003,348:593-600.
38.
WangJ,SimAS,WangXL,WilckenDE:L-arginineregulatesasymmetricdimethylargininemetabolismbyinhibitingdimethylargininedimethylaminohydrolaseactivityinhepatic(HepG2)cells.
CellularandMolecularLifeSciences2006,63(23):2838-46.
doi:10.
1186/1532-429X-12-50Citethisarticleas:Nguyenetal.
:Nasalcontinuouspositiveairwaypressureimprovesmyocardialperfusionreserveandendothelial-dependentvasodilationinpatientswithobstructivesleepapnea.
JournalofCardiovascularMagneticResonance201012:50.
SubmityournextmanuscripttoBioMedCentralandtakefulladvantageof:ConvenientonlinesubmissionThoroughpeerreviewNospaceconstraintsorcolorgurechargesImmediatepublicationonacceptanceInclusioninPubMed,CAS,ScopusandGoogleScholarResearchwhichisfreelyavailableforredistributionSubmityourmanuscriptatwww.
biomedcentral.
com/submitNguyenetal.
JournalofCardiovascularMagneticResonance2010,12:50http://www.
jcmr-online.
com/content/12/1/50Page10of10
Raksmart:香港高防服务器/20Mbps带宽(cn2+bgp)/40G-100Gbps防御
RAKsmart怎么样?RAKsmart香港机房新增了付费的DDoS高防保护服务,香港服务器默认接入20Mbps的大陆优化带宽(电信走CN2、联通和移动走BGP)。高防服务器需要在下单页面的IP Addresses Option里面选择购买,分:40Gbps大陆优化高防IP-$461/月、100Gbps国际BGP高防IP-$692/月,有兴趣的可以根据自己的需求来选择!点击进入:RAKsmart官...
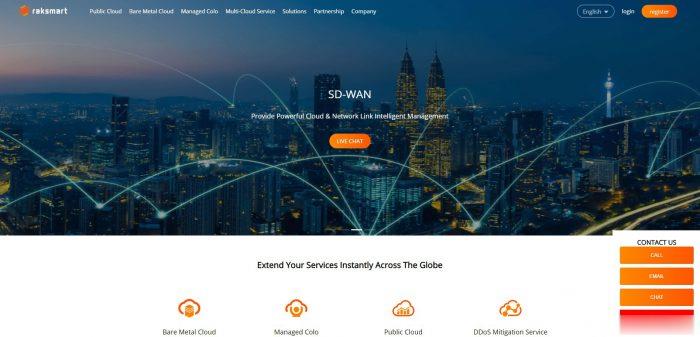
gcorelabs远东khabarovsk伯力Cloud云服务器测评,告诉你gcorelabs云服务器怎么样
说明一下:gcorelabs的俄罗斯远东机房“伯力”既有“Virtual servers”也有“CLOUD SERVICES”,前者是VPS,后者是云服务器,不是一回事;由于平日大家习惯把VPS和云服务器当做一回事儿,所以这里要特别说明一下。本次测评的是gcorelabs的cloud,也就是云服务器。 官方网站:https://gcorelabs.com 支持:数字加密货币、信用卡、PayPal...
LightNode($7.71/月)香港cn2精品线路
LightNode官网LightNode是一家位于香港的VPS服务商.提供基于KVM虚拟化技术的VPS.在提供全球常见节点的同时,还具备东南亚地区、中国香港等边缘节点.满足开发者建站,游戏应用,外贸电商等应用场景的需求。为用户带来高性能服务器以及优质的服务的同时还提供丰厚的促销活动,新用户注册最高送$20。注册用户带新客即可得10%返佣。商家支持PayPal,支付宝等支付方式。官网:https:/...
sebao为你推荐
-
宝来和朗逸哪个好大众朗逸好还是宝来好等额本息等额本金哪个好等额本金和等额本息哪个划算?如果想在5-10年内还清贷款哪类更划算一些?看书软件哪个好有什么好的读书软件啊?p图软件哪个好有什么P图工具比较好用dns服务器故障DNS服务器老是出错 如何从根本上解决??电信dns服务器地址广西电信应该填什么DNS服务器地址?360云盘下载360云盘和百度云哪个好用,请说出为什么。360云盘登陆怎样登陆360我的云盘强生月抛强生美瞳有月抛吗便宜坊便宜坊,4人去大概多少钱?